Same Day or Next Day Appointments Available Laredo (956) 726-9797 Se Habla Español
Same Day or Next Day Appointments Available Laredo (956) 726-9797 Se Habla Español
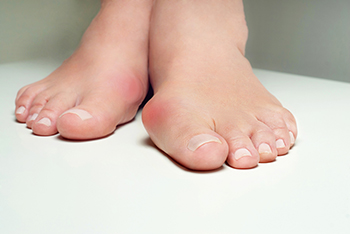
Bunions are bony protrusions at the base of the big toe that can not only be unsightly, but also painful. Managing bunions involves a combination of self care and professional guidance. Begin by wearing well-fitting shoes with ample room for your toes and avoiding high heels and pointy shoes that exacerbate pressure on the bunion. Taking over-the-counter pain relievers can provide temporary relief. Wearing custom orthotic inserts can alleviate discomfort by redistributing pressure. Regularly performing gentle toe stretches and exercises can improve flexibility and strength. In severe cases, surgical intervention may be considered. With a proactive approach, you can successfully manage bunions and maintain your foot health. If the bunion causes persistent pain or interferes with daily activities, it is suggested that you consult a podiatrist who can offer you additional relief and treatment methods.
If you are suffering from bunions, contact Jed Wells, DPM of Jed Wells, DPM Foot Specialist. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
If you have any questions, please feel free to contact our offices located in Corpus Christi, and Laredo, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.
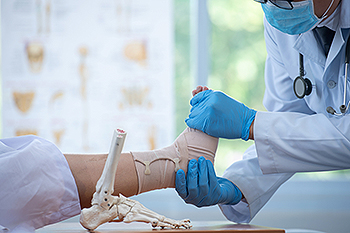
A bone fracture, such as an ankle fracture, occurs when a bone cracks or breaks due to high-force impact or stress. Even minor impacts can result in ankle fractures, especially in individuals with osteoporosis or bone cancer. An ankle fracture involves a complete or partial break in the ankle bone. Closed fractures spare surrounding tissue, while compound fractures break through the skin, raising infection risks. Fracture variations encompass avulsion, comminuted, compression, and more. Symptoms of a broken ankle differ based on age and injury severity and manifest as pain, swelling, bruising, and deformity. Causes of ankle fractures include trauma, overuse, and medical conditions. Age-related bone weakening and heightened disease susceptibility elevate fracture risk. Natural healing involves aligning and stabilizing the ankle bone with casts, plates, or rods. Healing duration depends on the fracture's severity and potential complications. Preventive measures include cautious exercising, proper diet, and addressing bone health, particularly during menopause. If you believe you have suffered a broken ankle, it is suggested that you make an appointment with a podiatrist for essential tests and treatment.
Broken ankles need immediate treatment. If you are seeking treatment, contact Jed Wells, DPM from Jed Wells, DPM Foot Specialist. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
Symptoms of a Fractured Ankle
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact our offices located in Corpus Christi, and Laredo, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The ankle is a hinged synovial joint made up of three bones: the tibia (shin bone), the fibula (outer ankle bone), and the talus (between the heel and leg). These three bones are bound, supported, and stabilized by strong, fibrous bands of tissue called ligaments.
A break in an ankle bone can be either traumatic or stress related. This injury may be referred to as a break or fracture. A traumatic fracture can result from tripping, twisting or rolling the ankle, falling, or by blunt impact to the ankle. These traumatic ankle breaks usually occur during sporting activities or accidents. Stress fractures, however, occur over time and are the result of repetitive stress to the ankle. These fractures sometimes occur when a new activity that engages the ankle is introduced, or when the level of activity is abruptly increased or intensified.
There are various symptoms that accompany an ankle break. The most significant symptoms are pain and swelling that occurs in the ankle and sometimes spreads up from the foot to below the knee. Bruising or discoloration may develop eventually. It will be difficult or even impossible to put weight on the affected foot, and in severe cases there may be a visible deformity or even exposed bone.
It is very important to seek immediate treatment when an ankle break occurs or is suspected to have occurred, in order to allow the bone to properly heal and to avoid future complications such as stiff joints, limited range of motion, and osteoarthritis.
To diagnose a broken ankle, your podiatrist will first ask you to explain how the injury occurred and what your symptoms are. They will perform a thorough examination, checking for damage to nerves, blood vessels, and other structures around the injury site. They will also test your range of motion. An X-ray will need to be reviewed and, in some cases, an MRI or CT scan may be necessary.
Proper treatment of a broken ankle will depend on where and how severe the break is, how stable the ankle is, and whether the bone is displaced (misaligned or separated) or non-displaced (broken yet still aligned properly).
Mild fractures (where the bone is non-displaced) may be treated by resting, icing, and elevating the ankle at first, followed by immobilization with a cast or walking boot. Pain and inflammation may be treated with acetaminophen. More severe or complicated fractures where bones or joints are displaced may require surgery.
Recovery time will also vary, and it may take 4-6 weeks or longer for a broken ankle to heal. Your podiatrist will most likely order progressive X-rays or stress tests to be taken in order to monitor the healing process.

The toes play a crucial role in our everyday movements, providing balance and stability. However, they are often overlooked when it comes to stretching and exercise routines. Just like any other part of our body, the toes can benefit from regular stretching to improve flexibility and prevent discomfort. Toe stretches can be simple yet effective, promoting blood circulation and relieving tension in the feet. One easy stretch involves sitting comfortably with feet flat on the floor and toes spread apart as much as possible. Hold this position for a few seconds and repeat it several times. Another beneficial stretch is gently pulling the toes back towards the body while keeping the foot flat on the ground. Regular toe stretching can be particularly beneficial for individuals who spend long hours on their feet, wear tight footwear, or suffer from conditions such as plantar fasciitis. If you would like additional information about various toe stretches, it is suggested that you consult with a podiatrist.
Why Stretching Is Important for Your Feet
Stretching the feet is a great way to prevent injuries. If you have any concerns with your feet consult with Jed Wells, DPM from Jed Wells, DPM Foot Specialist. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Stretching the Feet
Stretching the muscles in the foot is an important part in any physical activity. Feet that are tight can lead to less flexibility and make you more prone to injury. One of the most common forms of foot pain, plantar fasciitis, can be stretched out to help ease the pain. Stretching can not only ease pain from plantar fasciitis but also prevent it as well. However, it is important to see a podiatrist first to determine if stretching is right for you. Podiatrists can also recommend other ways to stretch your feet. Once you know whether stretching is right for you, here are some excellent stretches you can do.
It is best to go easy when first stretching your foot and work your way up. If your foot starts hurting, stop exercising to ice and rest the foot. It is advised that you then see a podiatrist for help.
If you have any questions, please feel free to contact our offices located in Corpus Christi, and Laredo, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Debilitating foot pain is a problem for many people. But just as stretching the torso can help alleviate back pain, stretching the feet can also help mend existing foot problems and prevent future ones.
The feet, as the body’s foundation, carry the body’s entire weight and can get easily strained from overexertion. Persistent sharp pain and cramping in the feet are often common concerns. Foot pain and foot problems can be due to any number of causes, and in many cases pain may be eased without medication or doctor visits. It is always a good idea, however, to first rule out any serious medical issues with a physician.
Stretching can help relax the feet and alleviate pain, but is especially important before heavy aerobic exercise. Stretching before such activities can help you avoid experiencing painful cramps or strained foot muscles. Stretches should be performed slowly and deliberately without forceful pulling. The stretch should be held for several seconds before relaxing.
A great way to stretch out and loosen up the foot muscles while sitting is to cross one leg over the other and pull the toes carefully back without overextending. Start by resting the left ankle on the right knee. With the left hand, gently flex the left foot by pulling back on the toes. Do not pull too hard; just hard enough to feel the stretch in the arch of the foot. Then point the toes of the left foot as far as you can. Rotate the motion of pointing with pulling back on the toes. This should relax and stretch the muscles on the bottom and the top of the foot. Doing this stretch ten to twenty times should bring relief. Repeat the whole process for the other foot by resting the right ankle on the left knee.
A stretch that focuses on the often injured Achilles tendon involves standing and facing a wall with your arms out and hands flat against the wall. Step back with one foot, keeping it flat against the floor. Move the other leg forward and lean toward the wall. You should feel a stretch through the back of your leg and your Achilles tendon, but do not push yourself too much. Stop when you feel a stretching sensation, and hold for 30 seconds. Ten repetitions may be done for each foot.
Stretching the feet is important for athletes or those performing aerobic exercise, but it can also help anyone with foot pain caused by poor footwear, plantar fasciitis, or long hours standing and walking. Individuals who tend to their feet by regularly stretching every day should be able to minimize foot pain and prevent new problems from arising.
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
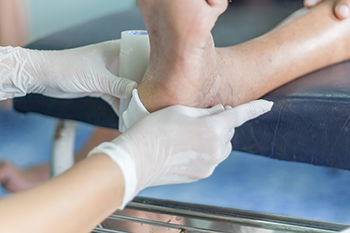
Pressure injuries on the heel bone, also called heel pressure ulcers, result from prolonged pressure and friction. The heel is the second most common site for such injuries due to its small area bearing the weight of the lower extremities. People with immobility, diabetes, leg spasms, or impaired blood flow are more susceptible to these injuries, affecting their quality of life. Prevention and healing involve alleviating pressure by using supportive devices. Such injuries can lead to open wounds, blisters, or deep tissue damage, increasing the risk of infection. Treatment options include pressure relief, proper wound care, specialized cushioning or boots, and, in severe cases, surgery. Due to the complexity and potential complications of such foot wounds, if you suffer from this, it is suggested that you make an appointment with a podiatrist for care.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Jed Wells, DPM from Jed Wells, DPM Foot Specialist. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Corpus Christi, and Laredo, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Our feet are arguably one of the most important parts of the body. When it comes to health and beauty routines, the feet and toenails are usually ignored. You should always practice proper footcare to avoid any fungal infections or ailments that can not only ruin the appearance of your feet, but also cause pain. Ignoring any foot problems could potentially lead to an expensive doctor’s visit.
The most important step in proper foot care is to wash your feet daily. You should wash them with soap and water. Doing this will cleanse your feet of dirt, sweat and bacteria. It is crucial that you clean between the toes and pat your feet dry with a towel afterward. Your toenails are also an important part of the feet and you may find that they get dirtier in the summer when you wear sandals. It is important that you practice proper toenail care in addition to cleaning the rest of your feet. When trimming your nails, you should always trim straight across instead of in a rounded shape. Trimming in a curved shape may lead to ingrown toenails.
Moisturization is also important for foot care, and you should be moisturizing your feet every day. The best way to prevent dry feet is to rub lotion or petroleum jelly on your clean feet at night and put socks over them. In the morning, your feet should be soft and moisturized.
Another crucial step in proper foot care is to wear the right shoes for whichever activity you are going to partake in. In warmer weather, you should wear shoes that allow your feet to breathe. It is best to avoid shoes such as flip-fops that do not provide arch support. Tight shoes may also be harmful, and they may even cause you to develop bunions.
If you plan on taking a shower in a public area, you should be especially careful, so you do not pick up any fungi. Showers are prone to harboring different types of bacteria and fungi. You should always wear shower shoes or flip flops when walking around in locker rooms and public showers. Avoid sharing shoes with other people because this is another way that fungus may be spread.
If you are experiencing any problems with your feet you should speak with your podiatrist to determine the best method of treatment for you.







